Research Whitepapers
Strategic Financial Impact Analysis of an Agentic AI Call Center for High-Volume Healthcare Systems
Executive Summary
Large healthcare systems face sustained pressure from rising patient access demand, persistent labor shortages, and escalating wage environments. High-volume call centers have become structurally expensive operating units, with cost profiles that scale linearly alongside call volume. Traditional cost controls, including headcount reductions and outsourcing, frequently degrade patient experience while introducing downstream revenue leakage from missed appointments and abandoned calls.
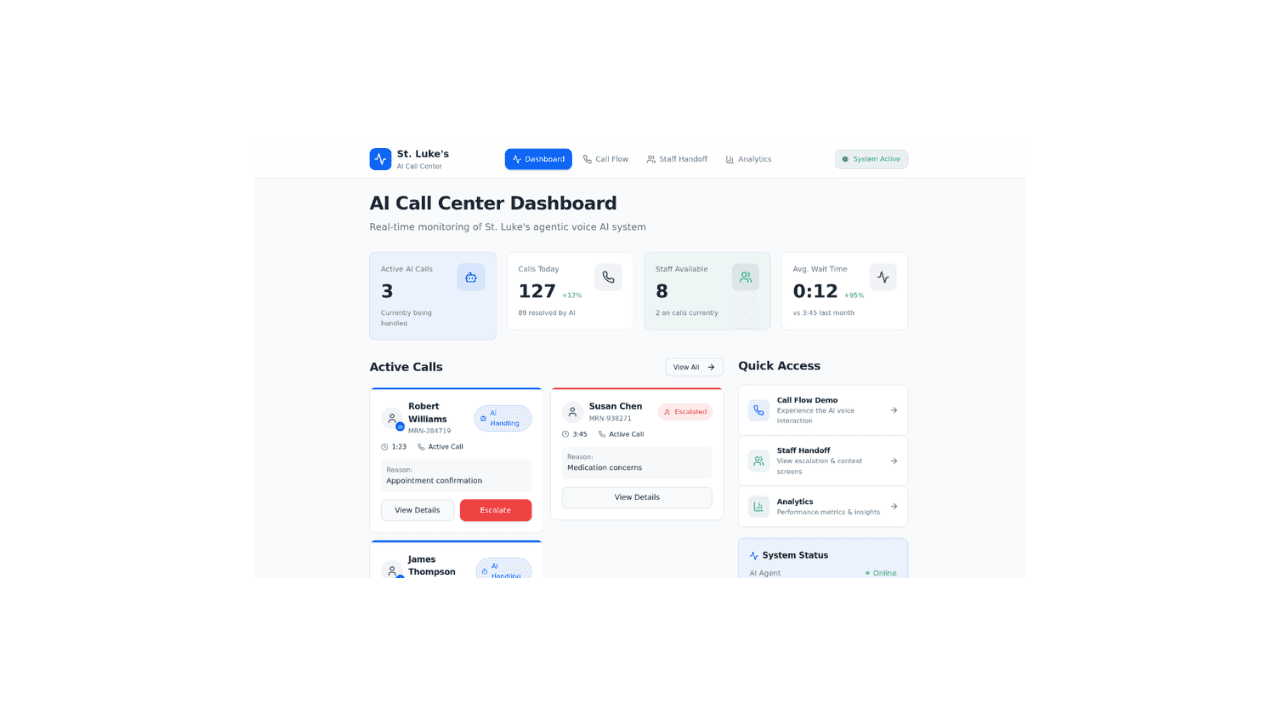
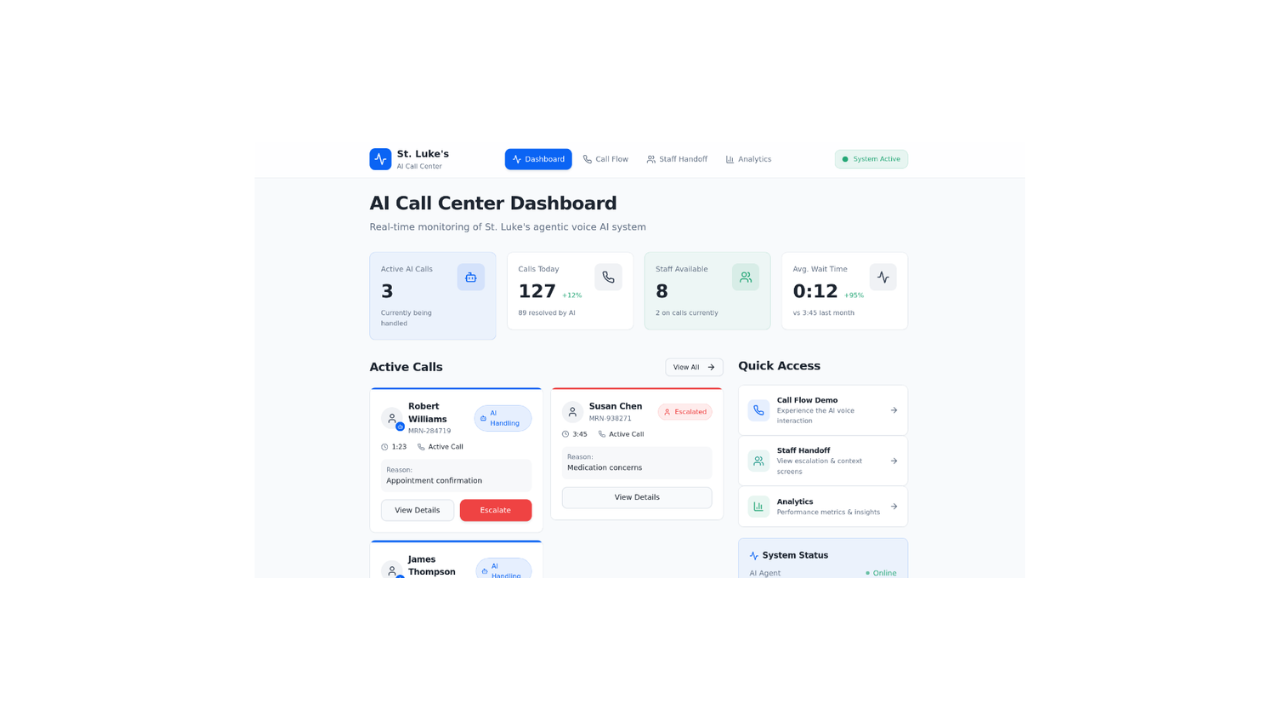
NextGen Coding Company evaluated an Agentic AI Call Center deployment for St. Luke’s Hospital, a multi-site health system processing approximately 400,000 inbound calls per month. The analysis demonstrates that agentic automation across prescription refills, appointment scheduling, and intake workflows can resolve approximately 70 percent of call volume autonomously while reducing average handle time for remaining human-assisted interactions.
At steady state, the operating model reduces required call center staffing from 781 full-time equivalents to 211 agents, generating projected net annual savings exceeding $28.7 million after cloud infrastructure costs. Over a ten-year horizon, cumulative net savings exceed $287 million while preserving service quality and clinical governance. Agentic AI converts the call center from a cost-intensive liability into a scalable operating asset without proportional headcount growth.
Problem Statement
Healthcare call centers operate under a structurally inefficient labor model. Every incremental increase in patient volume requires proportional increases in staffing, supervisory overhead, training, and physical infrastructure. In high-wage labor markets, staffing costs dominate the operating expense profile.
At St. Luke’s Hospital, inbound calls span prescriptions, appointment scheduling, clinical triage, and general inquiries. Prior to automation, all calls required human intervention, with average handle times of approximately 15 minutes per interaction. Manual HIPAA verification, redundant information gathering, and frequent inter-departmental transfers contributed to long queues, staff fatigue, and elevated abandonment risk.
Linear scaling under such conditions becomes financially unsustainable. Without structural change, patient access degradation becomes unavoidable as volumes rise.
Market and Regulatory Context
Healthcare contact centers operate under strict regulatory and clinical governance requirements. HIPAA, state privacy statutes, and internal risk management policies constrain outsourcing and limit aggressive offshoring strategies. Simultaneously, labor markets for healthcare support staff remain tight, with wage inflation outpacing reimbursement growth.
Agentic AI platforms have matured beyond traditional interactive voice response systems. Modern architectures combine speech recognition, natural language understanding, workflow orchestration, and EHR integration to resolve routine requests autonomously while preserving escalation pathways for clinical interactions.
Regulatory expectations increasingly favor auditable, deterministic automation over opaque outsourcing arrangements. AI-assisted workflows with full transcription, audit logging, and policy enforcement align more closely with compliance requirements than manual call routing models.
Methodology and Sources
The analysis uses operational inputs provided by St. Luke’s Hospital, supplemented by healthcare contact center benchmarks and published pricing from Amazon Web Services for managed AI services. Monthly call volume totals 400,000 interactions across patient access functions.
Evaluation Setup
Calculations assume a New York labor market with an average hourly wage of $22.00 and a fully burdened rate of $28.60 per hour inclusive of benefits and overhead. Agents operate on a 40-hour workweek with an effective utilization rate of 80 percent.
Automation coverage includes full resolution for prescription refills and appointment scheduling, representing 70 percent of total call volume. Remaining calls benefit from automated intake and pre-call context assembly.
Limitations
The analysis reflects steady-state performance following deployment ramp and optimization. Pilot-phase efficiency, seasonal volume variability, and potential incremental gains from advanced routing are excluded from base projections.
Reference Architecture or Approach
The Agentic AI Call Center architecture integrates managed speech-to-text, text-to-speech, conversational orchestration, analytics, and EHR connectivity. Core services include transcription, natural language processing, workflow agents, and call analytics operating within a HIPAA-aligned cloud environment.
Data Flow
Inbound calls are transcribed in real time, classified by intent, and routed to autonomous agents or human operators based on deterministic escalation policies. For clinical handoffs, structured summaries are delivered to providers prior to connection, reducing investigative overhead.
Tradeoffs
Managed cloud services accelerate deployment and compliance alignment but introduce variable usage costs. Custom model optimization offers future cost reductions at the expense of engineering complexity.
Implementation Guide
Deployment requires access to call metadata, EHR scheduling endpoints, prescription workflows, and clinical governance approval. Identity management and role-based access controls must integrate with existing hospital systems.
Deployment Steps
Initial rollout begins with pilot automation for low-risk workflows. Scheduling and prescription agents expand during subsequent phases, followed by optimization of intent classification and escalation thresholds.
Monitoring and Alerting
Real-time dashboards track automation rates, handle times, abandonment risk, and escalation frequency. Clinical oversight teams review flagged interactions for quality assurance.
Rollback and Restore
Manual routing remains available throughout deployment. Failover policies revert calls to human handling in the event of service degradation.
Deliverables
- Agentic workflow definitions
- EHR integration adapters
- Operational dashboards
- Governance and escalation policies
Evaluation and Benchmarks
Key Metrics
- Automation rate: 65–70 percent at steady state
- Average handle time reduction: 1.5 minutes per assisted call
- Monthly labor cost reduction: $2.6 million
- Annual net savings after cloud costs: $28.7 million
Benchmarks rely on explicit call volume, duration, wage, and pricing inputs. All calculations preserve units and published service rates.
Risks and Limitations
Operational risk centers on adoption pacing, staff training, and governance alignment. Overly aggressive automation thresholds may erode patient trust if escalation pathways remain unclear. Financial outcomes depend on sustained call volumes and disciplined scope control.
Case Example or Mini Study
St. Luke’s Hospital processes approximately 400,000 inbound calls monthly across multiple access functions, supported by a large human agent workforce.
Approach
Agentic AI resolved prescription refills and appointment scheduling autonomously while augmenting clinical calls with automated intake and summarization.
Measured Outcomes
Human-handled volume declined to 30 percent of total calls. Required staffing fell from 781 to 211 agents. Annual labor savings exceeded $31 million prior to cloud expenses.
Security, Privacy, and Compliance
Security controls align with HIPAA administrative, technical, and physical safeguards. Encryption protects data in transit and at rest. Role-based access controls restrict workflow execution. Full transcription and metadata logging support audit and retention policies. Data residency remains within United States regions.
Total Cost of Ownership (TCO) and Procurement Notes
Variables
- Call volume
- Average call duration
- Automation percentage
- Cloud service unit rates
Formulas
- Labor hours = calls × handle time ÷ 60
- Headcount = labor hours ÷ effective agent hours
- Net savings = labor reduction − cloud costs
Scenarios
- Conservative: 45–50 percent automation
- Base case: 65–70 percent automation
- Upside: 75–80 percent automation
Licensing and Support
Costs reflect managed cloud services without long-term licensing commitments. Support aligns with enterprise service-level agreements.
Exit Strategy and Portability
Architectural components support migration to alternative providers through standards-based APIs and data export mechanisms.
Glossary
- Agentic AI: Autonomous software agents capable of executing workflows without continuous human input
- AHT: Average handle time
- FHIR: Fast Healthcare Interoperability Resources
References
- Amazon Web Services pricing documentation
- HIPAA Security Rule guidance
- Healthcare contact center labor benchmarks
- AI-assisted patient access studies
- Cloud speech recognition performance analyses
- Call center workforce optimization research
- Healthcare automation governance frameworks
- EHR integration standards documentation
Call To Action
NextGen Coding Company designs resilient infrastructure that protects mission-critical communication at scale.
Contact admin@nextgencodingcompany.com or book a call to speak with our solutions team to begin scopinghttps://calendly.com/next_gen_coding_company/30min
Let’s Connect
At NextGen Coding Company, we’re ready to help you bring your digital projects to life with cutting-edge technology solutions. Whether you need assistance with AI, machine learning, blockchain, or automation, our team is here to guide you. Schedule a free consultation today and discover how we can help you transform your business for the future. Let’s start building something extraordinary together!